Timely Reminders to Access Prenatal Care

Context
Every year, more than 300,000 women and 2.5 million babies die from complications related to pregnancy and childbirth. The majority of these deaths occur in low-resource settings and in most cases could be prevented (WHO, 2016). Rural Guatemalans have little access to medical services, a fact that reduces the likelihood that women will receive adequate prenatal care.
In the mid-1990s, the Guatemalan government established the Coverage Extension Program (PEC) that provides free basic healthcare services to children under the age of five and to women of reproductive age, with a focus on preventive care. The Ministry of Health then hired local NGOs to operate a network of rural clinics in which health workers were expected to track individual families and inform them when to attend the monthly visits of the mobile medical team. There are no clear guidelines, however, and communication depends on the initiatives of health workers.
The Project
In an experimental intervention to improve uptake of prenatal care in low-resource settings, community healthcare workers in rural Guatemala were given up-to-date lists of pregnant women, enabling them to provide timely in-person reminders to attend clinics during visits from a mobile medical team.
Behavioral Analysis
Behavioral Barriers
Hassle factors: Seemingly small inconveniences, such as having to read a lot of information or take an extra small step to complete an action, can hinder or disrupt decision-making processes. Even when mothers are fully aware their children require vaccination, it takes only a few simple obstacles to deter them from following through.
Status quo bias: It is the tendency to maintain the current state of affairs, even when change is clearly better. This current status, or status quo, is used as a reference point, and any change with regard to this reference is seen as a loss. In this case, women may be reluctant to change their habits during pregnancy, such as visiting the clinic.
Present bias: It is the tendency to choose a smaller gain in the present over a large gain in the future. It is related to the preference for immediate gratification. It is also known as hyperbolic discounting. For example, women may skip a monthly prenatal visit even if that visit could prevent serious future health problems for their child.
Behavioral Tools
Reminders: They can take many forms, such as an email, a text message, a letter, or an in-person visit reminding individuals of some aspect of their decision-making process. Reminders are designed to mitigate procrastination, oversight, and cognitive overload.
Intervention Design
A sample of 130 clinics was randomly allocated to a treatment group and a control group. For those communities in the treatment group, community health workers received accurate and up-to-date information about pregnant women who would need prenatal care during the medical team’s upcoming visit to their clinic. Health workers were trained to use these lists to go house to house giving specific and timely in-person reminders to women so they would go to the clinic on the monthly visiting days. In the control group, the community health workers did not have the precise information of the program and had to rely on their own records.
Challenges
- To implement the intervention, PEC designers developed a software program that generated the lists of patients from the program’s medical record system; these were delivered to the community health workers during their monthly meeting with the NGO.
- Pregnant women received a prenatal checkup during which weight, blood pressure, and abdominal circumference were measured. Urine samples were taken, and the women were given prenatal vitamins and food supplements. A smaller proportion of the population within the treatment group received tetanus vaccines and ultrasounds to assess the baby’s health.
Results
The reminders had a positive and statistically significant effect on prenatal checkups six months before delivery, increasing their probability by 6.6 percentage points. The first trimester of pregnancy is significant for fetal development, so these prenatal checkups are particularly important. We also find positive and statistically significant effects on prenatal assessments one and two months before delivery (7.8 and 7.2 percentage points, respectively).
Treatment effects increase with age. For women between ages 14 and 24 years, the effect was small and statistically insignificant. The intervention increases the probability of women aged 25 to 35 years of getting a prenatal checkup one month before delivery by 11.4 percentage points. The effect is even greater for women between 36 and 49 years of age (47.9 percentage points). Intervention effects are also larger and statistically significant for women who had had one previous miscarriage and for women pregnant for the first time. In sum, the intervention seems to be more effective for the group of women who would benefit most from regular prenatal checkups.
Figure 1. Prenatal control attendance
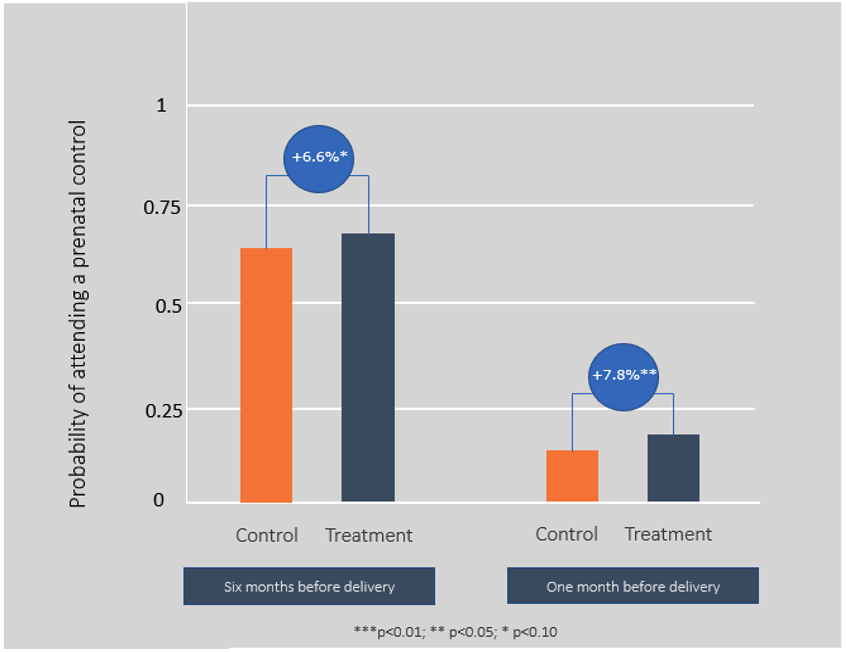
Policy Implications
- The project offers evidence that reminders play a promising role in demand for preventive health services. There is an opportunity to expand the role of reminders to achieve further gains in prenatal healthcare rates at a moderate cost.
